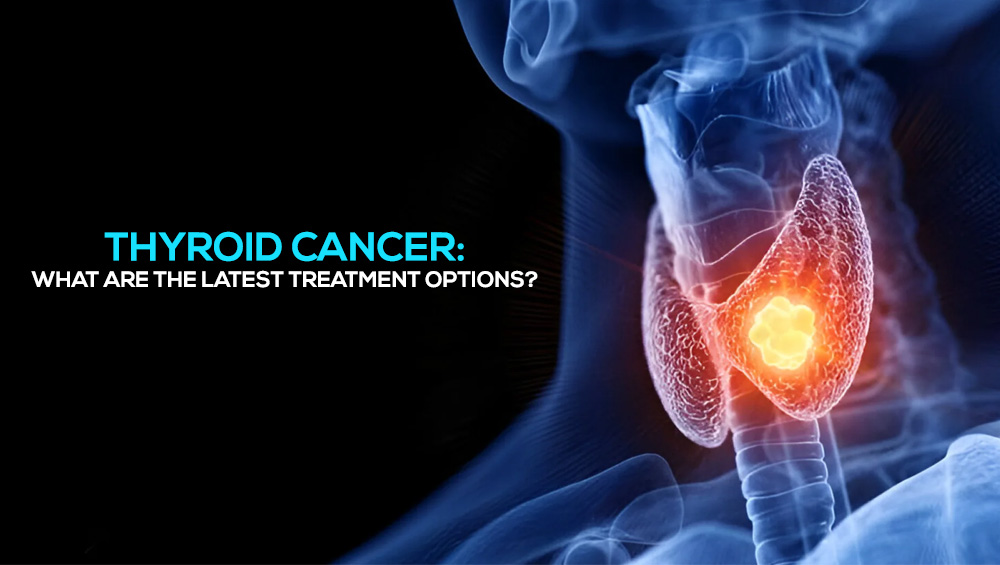
Thyroid cancer is a disease in which malignant (cancerous) cells form in the tissues of the thyroid gland, a butterfly-shaped organ located at the base of the neck. The thyroid gland produces hormones that regulate metabolism, heart rate, and body temperature.
Thyroid cancer is generally highly treatable and often curable, with a five-year survival rate exceeding 98%.
Risk Factors for Thyroid Cancer
Several factors may increase the risk of developing thyroid cancer:
Age and Gender
- Age over 50 years carries a higher risk
- Women are more frequently affected than men
Genetic Conditions
- Certain inherited syndromes such as MEN 2, familial adenomatous polyposis, and Cowden syndrome
Family History
- Having first-degree relatives (parents, siblings, or children) with thyroid cancer
Radiation Exposure
- Exposure during childhood for other medical conditions (e.g., childhood lymphoma, sarcoma, etc.)
Low Iodine Intake
- Associated with a higher risk of developing papillary and follicular thyroid cancers
Different Types of Thyroid Cancer
Thyroid cancer is categorized based on the type of cells from which the cancer originates and how closely those cells resemble normal thyroid tissue (degree of differentiation).
1. Differentiated Thyroid Cancers (DTC)
These cancers arise from follicular cells, which produce thyroid hormone.
- Papillary Thyroid Cancer:The most common type, accounting for 80–90% of all thyroid cancers. It is usually slow-growing and highly curable.
- Follicular Thyroid Cancer:Accounts for 10–15% of cases. It is more likely than papillary cancer to spread through the bloodstream to distant organs such as the lungs or bones.
- Hürthle Cell (Oncocytic) Cancer:A rarer form (approximately 3%) that is often more aggressive and less responsive to radioactive iodine therapy.
2. Medullary Thyroid Cancer (MTC)
Medullary thyroid cancer accounts for approximately 2–5% of cases and arises from C-cells (parafollicular cells), which produce calcitonin rather than thyroid hormone.
- Hereditary Risk:About 25% of cases are inherited through genetic mutations (e.g., RET gene) and may be associated with Multiple Endocrine Neoplasia type 2 (MEN2).
- Treatment Difference:MTC does not respond to radioactive iodine or thyroid-stimulating hormone (TSH) suppression therapy.
3. Anaplastic Thyroid Cancer (ATC)
A highly aggressive and undifferentiated cancer, accounting for 1–2% of cases. The cancer cells look very different from normal thyroid cells and grow rapidly.
4. Rare and Other Types
- Poorly Differentiated Thyroid Cancer:An uncommon type with behavior between differentiated and anaplastic cancers.
- Thyroid Lymphoma:A very rare cancer (1–2%) arising from lymphoid tissue within the thyroid.
- Thyroid Sarcoma:An extremely rare cancer originating from muscles, nerves, or blood vessels of the thyroid.
Thyroid Cancer: The Indian Scenario
In 2025, thyroid cancer in India shows a significant rise in incidence, particularly among women in urban areas. This increase is largely attributed to improved diagnostic detection. In some regions, it is now the fifth most common cancer among Indian women.
Incidence and Demographic Trends
- Rising Incidence:The current incidence rate is approximately 5.4 per lakh population.
- Gender and Age:Women are more commonly affected than men, with a female-to-male ratio of approximately 2.1:1, rising to 4.3:1in individuals under 35 years of age.The peak age of diagnosis is between 30 and 50 years.
Histological Profile
- Papillary Thyroid Carcinoma (PTC):The most common subtype, accounting for 69–92% of cases. It is slow-growing and highly treatable.
- Other Types:Follicular carcinoma (~11%), medullary carcinoma (~4.5%), and anaplastic carcinoma (~2.6%).
Despite the rising incidence, the mortality rate remains low and stable, approximately 0.4–0.7 per 100,000 women. Differentiated thyroid cancers have an excellent prognosis, with five-year survival rates exceeding 95–98% when detected early.
Thyroid Cancer Treatment Options
By 2025, thyroid cancer treatment in India has become highly advanced, combining surgical expertise with molecular and targeted therapies. Treatment is individualized based on cancer type and stage.
1. Surgical Interventions (Cornerstone of Treatment)
Surgery remains the primary treatment modality.
- Total Thyroidectomy:Complete removal of the thyroid gland, recommended for large or aggressive tumours.
- Total Thyroidectomy with Central Compartment Clearance:Removal of lymph nodes in the central neck region along with the thyroid gland, improving disease control and staging.
- Lobectomy (Hemithyroidectomy):Removal of one thyroid lobe and isthmus, suitable for low-risk tumours confined to one lobe.
- Lymph Node Dissection:Removal of involved lymph nodes when cancer spread is detected.
- Robotic Thyroid Surgery:A minimally invasive technique available in major Indian metro hospitals that avoids visible neck scars by accessing the gland through the armpit, ear, or mouth.
2. Radioactive Iodine Therapy (I-131)
Commonly used after surgery for papillary and follicular thyroid cancers.
- Mechanism:I-131 selectively destroys remaining thyroid or cancer cells.
- Availability:Provided at specialized nuclear medicine centres, requiring short-term isolation (usually 1–3 days).
3. Thyroid Hormone Suppression Therapy
- Hormone Replacement:Lifelong thyroid hormone therapy (e.g., levothyroxine) is required after surgery.
- Cancer Control:Higher doses are often used to suppress TSH, which can stimulate cancer cell growth.
4. Targeted and Systemic Therapies
Used for advanced, metastatic, or radioactive iodine–refractory disease.
- Multikinase Inhibitors:Lenvatinib and Sorafenib
- Specific Targeted Drugs:Selpercatinib, Pralsetinib (RET mutations)Dabrafenib + Trametinib (BRAF-mutated anaplastic cancer)
- External Beam Radiation Therapy (EBRT):Used for inoperable or aggressive cancers
- Immunotherapy:Considered in select treatment-resistant cases
5. Thyroid Ablation
Minimally invasive alternatives to surgery are increasingly used in India.
- Radiofrequency Ablation (RFA)
- Microwave Ablation (MWA)
- Laser Ablation (LA)
When Is Ablation Used?
- Benign symptomatic nodules
- Low-risk papillary microcarcinomas (<1 cm)
- Recurrent thyroid cancer when surgery is high risk
Advantages of Thyroid Ablation
- Performed under local anaesthesia as a day-care procedure
- No visible scar
- Preserves healthy thyroid tissue
- Often avoids lifelong hormone replacement
- Procedure duration: 30–60 minutes
6. Active Surveillance
For very small, low-risk papillary microcarcinomas, Indian guidelines now support active surveillance, involving regular ultrasound monitoring without immediate surgery to avoid overtreatment.