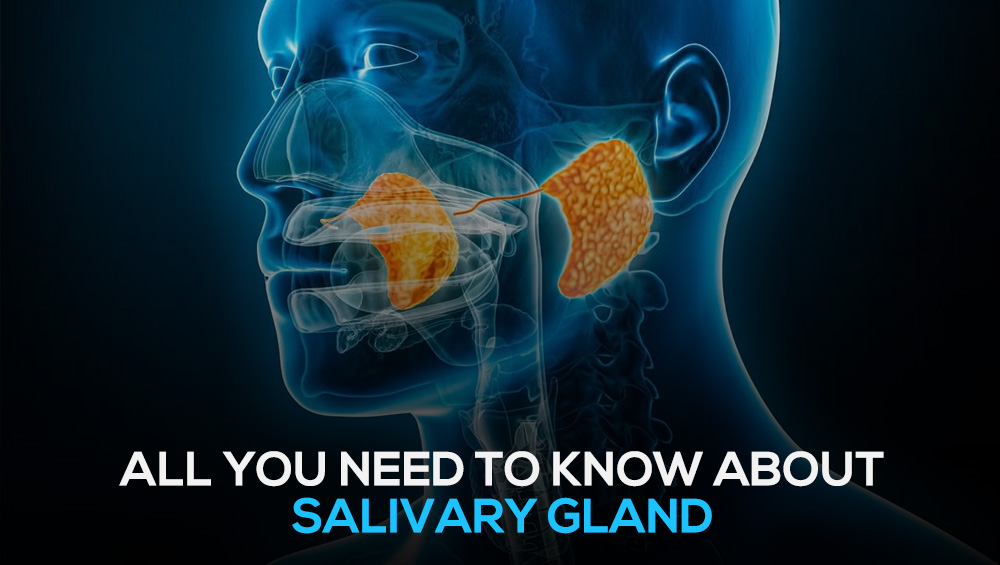
Tumours of the salivary glands are a diverse group of tumours originating from the major salivary glands—parotid, submandibular, and sublingual—or from the thousands of minor salivary glands located throughout the upper aerodigestive tract. These tumours represent approximately 3–6% of all head and neck neoplasms.
Epidemiology and General Patterns
Distribution
- Most salivary gland tumours (70–85%) occur in the parotid gland
- Approximately 80% of parotid tumours are benign
Rule of Proportion
A key clinical rule is that the smaller the gland of origin, the higher the risk of malignancy:
- Parotid gland: ~20–25% malignant
- Submandibular gland: ~40–50% malignant
- Sublingual & minor salivary glands: ~70–90% malignant
Classification
(**World Health Organization – WHO 5th Edition, 2022/2024)
Common Benign Neoplasms
- Pleomorphic Adenoma (Benign Mixed Tumour)
- The most common salivary gland tumour overall
- Represents approximately 60–70% of parotid neoplasms
- Warthin Tumour (Papillary Cystadenoma Lymphomatosum)
- Second most common benign tumour
- Almost exclusively found in the parotid gland
- Strongly associated with smoking
- 10% are bilateral, affecting both glands simultaneously
- Basal Cell Adenoma
- Rare, usually encapsulated benign tumour
- Most commonly seen in the parotid gland
Common Malignant Neoplasms
- Mucoepidermoid Carcinoma (MEC)
- The most common salivary gland malignancy
- Adenoid Cystic Carcinoma (ACC)
- Most commonly affects submandibular and minor salivary glands
- High risk of local invasion and distant metastasis
- Acinic Cell Carcinoma
- Indolent, low-grade tumour
- Most commonly occurs in the parotid gland
- Polymorphous Adenocarcinoma
- Commonly found in minor salivary glands, especially the palate
Clinical Presentation
Most salivary gland tumours present as a painless, slow-growing mass.
“Red Flag” Symptoms Suggesting Malignancy
- Facial nerve paralysis: weakness on one side of the face
- Pain: often indicates rapid growth or secondary infection
- Fixation: hard mass adherent to overlying skin
- Lymphadenopathy: swollen lymph nodes in the neck
Diagnosis and Management
1. Imaging
- MRI: preferred imaging modality
- CT scan: useful for assessing bone involvement
- PET-CT scan: may be used in confirmed malignancy
2. Biopsy
- Fine-needle aspiration (FNA): commonly used for preliminary diagnosis and surgical planning
- Definitive diagnosis: usually established after surgical excision
3. Surgery
Surgery is the primary treatment for both benign and malignant salivary gland tumours.
Surgical Procedures
1. Parotidectomy
Surgical removal of part or all of the parotid gland. Primarily performed for tumours but may also be used for chronic infections, salivary stones, or sialadenitis.
Types of Parotidectomy
- Superficial Parotidectomy:Removal of the superficial lobe (lateral to the facial nerve); most common procedure
- Total Parotidectomy:Removal of both superficial and deep lobes, usually for deep-lobe or extensive tumours
- Radical Parotidectomy:Removal of the entire gland along with the facial nerve, indicated in aggressive malignancies involving the nerve
2. Submandibular Gland Surgery (Submandibular Gland Excision)
Removal of one or both submandibular glands, commonly performed for stones, chronic infection, or tumours.
Indications for Surgery
- Tumours: approximately 40–50% are malignant
- Salivary stones (sialolithiasis)
- Chronic inflammation: including Kuttner’s tumour or autoimmune disorders unresponsive to conservative treatment
3. Neck Dissection
Performed when lymph node metastasis is present in malignant disease.
Adjuvant Therapy
Postoperative radiotherapy is indicated for:
- High-grade tumours
- Advanced-stage disease
- Recurrent cancers
Risks and Complications of Salivary Gland Surgery
- Nerve weakness or numbness: temporary lower lip weakness, earlobe or tongue numbness
- Hematoma or seroma: blood or fluid collection requiring drainage
- Infection: uncommon
- Dry mouth
- Facial weakness or paralysis: temporary weakness common; permanent paralysis rare
- Frey’s syndrome: facial sweating or flushing during eating
- Salivary fistula or sialocele: leakage or collection of saliva at the surgical site
Reconstructive Surgery of the Facial Nerve
Facial reanimation is a specialized field focused on restoring facial tone, symmetry, and voluntary movement.
Dynamic Reanimation (Movement Restoration)
Aimed at restoring active facial movements such as smiling or eye closure.
Nerve Repair and Grafting (Within 12–18 Months)
- Primary nerve repair
- Cable grafting
- Nerve transfers (crossover)
- Cross-facial nerve graft
Functional Muscle Transfer (After 12–18 Months)
- Gracilis free flap
- Temporalis tendon transfer
Static Procedures (Symmetry and Protection)
These procedures improve facial appearance at rest and protect vital functions.
Eye Protection
- Eyelid weights
- Tarsorrhaphy / Canthoplasty
Symmetry Restoration
- Static slings
- Brow lift and face lift